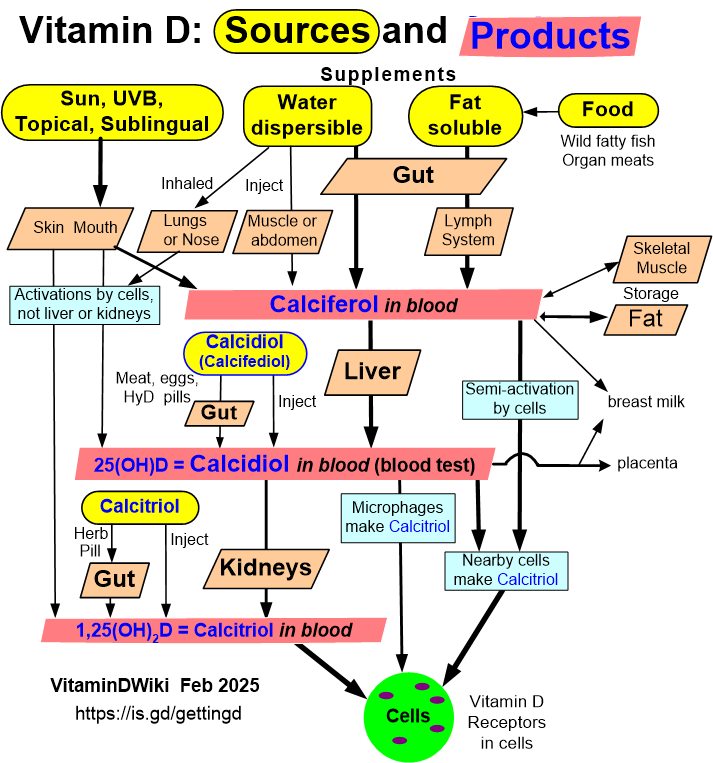
Perhaps 80% of Vitamin D activation is done by cells (not kidneys)
What Heaney actually said (back in 2008) - Claude AI May 2026
In his Clin J Am Soc Nephrol review "Vitamin D in Health and Disease," Heaney wrote that vitamin D functions through both an endocrine mechanism (regulating calcium absorption) and an autocrine mechanism (facilitating gene expression), and that the autocrine pathway "accounts for more than 80% of the metabolic utilization of the vitamin each day, produces, uses, and degrades calcitriol exclusively intracellularly." The reasoning was a flux argument: only a small fraction of daily 25(OH)D turnover can be accounted for by the renal calcitriol that ends up in serum; the rest must be consumed somewhere, and the candidate is intracrine activation in extrarenal tissues. The "half" figure you recall was probably a more cautious paraphrase that floated around the same period.
Why no new number has replaced it
You can measure renal output reasonably well, because renal calcitriol goes into the bloodstream where it can be sampled. But extrarenal calcitriol is consumed inside the same cell that made it — degraded by CYP24A1 before it ever leaves — so there's no body-fluid compartment in which to measure it. To produce a real quantitative estimate, you'd need either:
- a stable-isotope flux study in humans tracking total 25(OH)D → 1,25(OH)₂D conversion in vivo, or
- tissue-level mass balance from biopsies across many organs.
Neither has been done at the whole-body level. As a result, every recent review still cites Heaney 2008 or speaks qualitatively. Pike and Christakos in their 2020 J Clin Invest "Unsettled Science" Viewpoint were explicit that "although local production of calcitriol in NRTCs has gained wide acceptance in the field, key fundamental insights supporting the relevance of this process and its biological consequences remain outstanding."
What the 2020–2025 literature now says
The newest authoritative review — Zittermann, Int J Mol Sci 26: 5570 (June 2025) — does not give a body-wide percentage. It accepts that extrarenal CYP27B1 is widely distributed and that locally synthesized calcitriol is "largely degraded before it enters the circulation," but it then introduces an important wrinkle that pushes back somewhat against the simple Heaney/Hollis substrate-driven picture:
Immune cells appear NOT to be straightforwardly substrate-limited. Zittermann concludes that "calcitriol synthesis in immune cells is obviously not primarily dependent on circulating 25-hydroxyvitamin D, which challenges the use of vitamin D for infection prevention." His evidence: macrophage CYP27B1 is dominated by TLR/IFN-γ/IL-15 signaling and is suppressed by FGF23 (which is elevated in CKD and heart failure), so the limiting factor is not always 25(OH)D supply.
The placenta and granulomatous macrophages remain the only extrarenal sites whose output spills into serum. Everywhere else, the extrarenal flux is real but invisible to standard assays.
- Most "in healthy adults" calcitriol regulation is still renal, driven by PTH/FGF23/Ca²⁺/Pi.
So what's the current best guess?
The most defensible summary as of 2026:
- In terms of where 25(OH)D molecules end up being activated to calcitriol — Heaney's >80% extrarenal estimate has not been overturned and is still the only quantitative figure in wide circulation. The Hollis/Wagner, Hewison, Bikle, Holick, and Carlberg camps essentially endorse it. Most of the body's daily calcitriol production (counting intracellular events) is extrarenal.
- In terms of where calcitriol that enters the bloodstream comes from — the answer is still ~99% renal in non-pregnant adults without granulomatous disease.
- In terms of biological importance — at least half, probably most, of vitamin D's clinically relevant effects depend on extrarenal/intracrine activation. This is the central rationale for measuring 25(OH)D rather than 1,25(OH)₂D and for keeping serum 25(OH)D well above the skeletal-sufficiency threshold.
What's changed in the last decade is not the number but the conviction. In 2008 Heaney's >80% was a provocative claim against an entrenched kidney-centric view; by 2025 it's the consensus working model, just without a tighter number behind it. The next real advance will probably come from stable-isotope kinetic studies, and as far as I can find, none has been published.
Related in VitaminDWiki
- 35 tissues activate Vitamin D locally (Kidney not required): cancers (4+), reproductive, lungs, skin, etc.
3 Types of Vitamin D